Managing Fallen Arches

A person with flat feet (fallen arches) has low arches or no arches at all. Most cases don't cause problems and treatment isn't usually needed. The arch, or instep, is the inside part of the foot that's usually raised off the ground when you stand, while the rest of the foot remains flat on the ground. Most people have a noticeable space on the inner part of their foot (the arch). The height of the arch varies from person to person.
Causes
Flat feet in adults can appear for a number of reasons. Arches never developed properly. Damage to the tendons that support the arch. Damage or inflammation of the posterior tibial tendon which runs from your lower leg, down and across your ankle, and connects to the middle of the arch. Trauma involving broken bones in the foot. Rheumatoid arthritis. Aging, pregnancy, nerve damage, obesity or even diabetes.
Symptoms
People will have a very heavily dropped arch and it won?t affect them at all and people will have it slightly dropped and it could cause fierce problems. It could cause things like plantar fasciitis, it could cause heel spurs, desperate ball-of-the-foot pressure, or pressure on the big toe known as the hallux which causes discomfort in the foot. It will create problems upwards to the knees, hips and the back once you?re out of line.
Diagnosis
Diagnosis of flat feet or fallen arches can be made by your health practitioner and is based on the following. Clinical assessment involving visual gait assessment, as well as biomechanical assessment. A detailed family and medical history. A pain history assessment determining the location of painful symptoms. Physical palpation of the feet and painful areas. Imaging such as MRI or x-ray can be used by your practitioner to assist in the diagnosis.
deelsonheels
Non Surgical Treatment
Flexible flat feet that are painless do not require treatment. If you have pain due to flexible flat feet, an orthotic (arch-supporting insert in the shoe) can bring relief. With the increased interest in running, many shoe stores carry shoes for normal feet and pronated feet. The shoes designed for pronated feet make long distance running easier and less tiring because they correct for the abnormality. Rigid or painful flat feet require evaluation by a health care provider. The treatment depends on the cause of the flat feet. For tarsal coalition, treatment starts with rest and possibly a cast. If this fails to improve the pain, surgery may be necessary. For problems with the posterior tibial tendon, treatment may start with rest, anti-inflammatory medications, and shoe inserts or ankle braces. In more advanced cases, surgery may be needed to clean or repair the tendon, or fuse some of the joints of the foot into a corrected position. Flat feet in older adults can be treated with pain relievers, orthotics, and sometimes surgery.
Surgical Treatment

Surgery for flat feet is separated into three kinds: soft tissue procedures, bone cuts, and bone fusions. Depending on the severity of the flat foot, a person?s age, and whether or not the foot is stiff determines just how the foot can be fixed. In most cases a combination of procedures are performed. With flexible flat feet, surgery is geared at maintaining the motion of the foot and recreating the arch. Commonly this may involve tendon repairs along the inside of the foot to reinforce the main tendon that lifts the arch. When the bone collapse is significant, bone procedures are included to physically rebuild the arch, and realign the heel. The presence of bunions with flat feet is often contributing to the collapse and in most situations requires correction. With rigid flat feet, surgery is focused on restoring the shape of the foot through procedures that eliminate motion. In this case, motion does not exist pre-operatively, so realigning the foot is of utmost importance. The exception, are rigid flat feet due to tarsal coalition (fused segment of bone) in the back of the foot where freeing the blockage can restore function.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.
What Are The Major Causes Of Heel Discomfort

The heel is the first bone to contact the ground when walking and takes the full force of impact and the resulting shock of bearing weight during motion. The primary symptom is pain in the heel area that varies in severity and location. The pain is commonly intense when getting out of bed or a chair. The pain often lessens when walking. The most common cause of heel pain is plantar fasciitis. Plantar fasciitis is a stretching of the plantar fascia, a ligament that runs from the ball of foot through the arch and is attached to the heel. It is that attachment which becomes aggravated and typically causes pain after being on your feet for lengths of time. Abnormal motion of the foot (pronation) is one cause of plantar fasciitis. Heel spurs, which are abnormal bone growths coming off the heel, can also cause heel pain. Other causes include repetitive stress or shock to the heel, standing for prolonged periods or osteoarthritis. To prevent heel pain, always wear properly fitting shoes, place insoles or inserts in your shoes to help control abnormal foot motion, maintain a healthy weight, exercise and do foot stretches as they have been shown to decrease the incidence of heel pain.
Causes
Heel pain is most often the result of overuse. Rarely, it may be caused by an injury. Your heel may become tender or swollen from, shoes with poor support or shock absorption. Running on hard surfaces, like concrete. Running too often. Tightness in your calf muscle or the Achilles tendon. Sudden inward or outward turning of your heel. Landing hard or awkwardly on the heel. Conditions that may cause heel pain include. When the tendon that connects the back of your leg to your heel becomes swollen and painful near the bottom of the foot. Swelling of the fluid-filled sac (bursa) at the back of the heel bone under the Achilles tendon (bursitis). Bone spurs in the heel. Swelling of the thick band of tissue on the bottom of your foot (plantar fasciitis). Fracture of the heel bone that is related to landing very hard on your heel from a fall (calcaneus fracture).
Symptoms
The symptoms of plantar fasciitis are classically pain of a sharp nature which is worse standing first thing in the morning. After a short period of walking the pain usually reduces or disappears, only to return again later in the day. Aggravating times are often after increased activity and rising from sitting. If these are the sort of symptoms you are experiencing then the Heel-Fix Kit ? will be just the treatment your heel is crying out for. Some heel pain is more noticeable at night and at rest. Because plantar fasciitis is a mechanical pathology it is unlikely that this sort of heel pain is caused by plantar fasciitis. The most common reason for night heel pain is pressure on your Sciatic nerve causing referred pain in the heel. Back pain is often present as well, but you can get the heel pain with little or no back pain that is caused by nerve irritation in the leg or back. If you get pain in your heels mainly or worse at night please see a clinician as soon as you can to confirm the diagnosis.
Diagnosis
Your GP or podiatrist (a healthcare professional who specialises in foot care) may be able to diagnose the cause of your heel pain by asking about your symptoms and examining your heel and foot. You will usually only need further tests if you have additional symptoms that suggest the cause of your heel pain is not inflammation, such as numbness or a tingling sensation in your foot - this could be a sign of nerve damage in your feet and legs (peripheral neuropathy), your foot feels hot and you have a high temperature (fever) of 38C (100.4F) or above - these could be signs of a bone infection, you have stiffness and swelling in your heel - this could be a sign of arthritis. Possible further tests may include, blood tests, X-rays - where small doses of radiation are used to detect problems with your bones and tissues, a magnetic resonance imaging (MRI) scan or ultrasound scan, which are more detailed scans.
Non Surgical Treatment
Home care, in cases that are not severe, home care is probably enough to get rid of heel pain. Rest, avoid running or standing for long periods, or walking on hard surfaces. Avoid activities that may stress the heels. Ice, place an ice-pack on the affected area for about 15 minutes. Do not place bare ice directly onto skin. Footwear. proper-fitting shoes that provide good support are crucial. Athletes should be particularly fussy about the shoes they use when practicing or competing - sports shoes need to be replaced at specific intervals (ask your trainer). Foot supports, wedges and heel cups can help relieve symptoms.
Surgical Treatment
With the advancements in technology and treatments, if you do need to have surgery for the heel, it is very minimal incision that?s done. And the nice thing is your recovery period is short and you should be able to bear weight right after the surgery. This means you can get back to your weekly routine in just a few weeks. Recovery is a lot different than it used to be and a lot of it is because of doing a minimal incision and decreasing trauma to soft tissues, as well as even the bone. So if you need surgery, then your recovery period is pretty quick.
heel cups for heel pain
Prevention

Make sure you wear appropriate supportive shoes. Don't over-train in sports. Make sure you warm up, cool down and undertake an exercise regime that helps maintain flexibility. Manage your weight, obesity is a factor in causing plantar fasciitis. Avoid walking and running on hard surfaces if you are prone to pain. You should follow the recognized management protocol "RICED" rest, ice, compression, elevation and diagnosis. Rest, keep off the injured ankle as much as possible. Ice, applied for 20 minutes at a time every hour as long as swelling persists. Compression, support the ankle and foot with a firmly (not tightly) wrapped elastic bandage. Elevation, keep foot above heart level to minimize bruising and swelling. Diagnosis. Consult a medical professional (such as a Podiatrist or doctor) especially if you are worried about the injury, or if the pain or swelling gets worse. If the pain or swelling has not gone down significantly within 48 hours, also seek treatment. An accurate diagnosis is essential for proper rehabilitation of moderate to severe injuries.
Leg Length Discrepancy Shoe Inserts
There are many different conditions in childhood and adult life that can lead to deformity of a limb or difference in leg lengths. Treatment for these conditions depends on the condition being treated, the age of the child and the amount of deformity or shortening. Generally, only a final difference of leg length of 2cm or more requires surgical treatment. An outline of treatment options is given below.
.png)
Causes
Some causes of leg length discrepancy (other than anatomical). Dysfunction of the hip joint itself leading to compensatory alterations by the joint and muscles that impact on the joint. Muscle mass itself, i.e., the vastus lateralis muscle, pushes the iliotibial band laterally, causing femoral compensations to maintain a line of progression during the gait cycle. This is often misdiagnosed as I-T band syndrome and subsequently treated incorrectly. The internal rotators of the lower limb are being chronically short or in a state of contracture. According to Cunningham's Manual of Practical Anatomy these are muscles whose insertion is lateral to the long axis of the femur. The external rotators of the hip joint are evidenced in the hip rotation test. The iliosacral joint displays joint fixations on the superior or inferior transverse, or the sagittal axes. This may result from many causes including joint, muscle, osseous or compensatory considerations. Short hamstring muscles, i.e., the long head of the biceps femoris muscle. In the closed kinetic chain an inability of the fibula to drop inferior will result in sacrotuberous ligament loading failure. The sacroiliac joint dysfunctions along its right or left oblique axis. Failure or incorrect loading of the Back Force Transmission System (the longitudinal-muscle-tendon-fascia sling and the oblique dorsal muscle-fascia-tendon sling). See the proceedings of the first and second Interdisciplinary World Congress on Low Back Pain. Sacral dysfunction (nutation or counternutation) on the respiratory axis. When we consider the above mentioned, and other causes, it should be obvious that unless we look at all of the causes of leg length discrepancy/asymmetry then we will most assuredly reach a diagnosis based on historical dogma or ritual rather than applying the rules of current differential diagnosis.
Symptoms
Many people walk around with LLD?s of up to 2 cm. and not even know it. However, discrepancies above 2 cm. becomes more noticeable, and a slight limp is present. But even up to 3 cm. a small lift compensates very well, and many patients are quite happy with this arrangement. Beyond 3 cm. however, the limp is quite pronounced, and medical care is often sought at that point. Walking with a short leg gait is not only unsightly, but increases energy expenditure during ambulation. It could also put more stress on the long leg, and causes functional scoliosis. Where the discrepancy is more severe, walking becomes grotesque or virtually impossible.
Diagnosis
The most accurate method to identify leg (limb) length inequality (discrepancy) is through radiography. It?s also the best way to differentiate an anatomical from a functional limb length inequality. Radiography, A single exposure of the standing subject, imaging the entire lower extremity. Limitations are an inherent inaccuracy in patients with hip or knee flexion contracture and the technique is subject to a magnification error. Computed Tomography (CT-scan), It has no greater accuracy compared to the standard radiography. The increased cost for CT-scan may not be justified, unless a contracture of the knee or hip has been identified or radiation exposure must be minimized. However, radiography has to be performed by a specialist, takes more time and is costly. It should only be used when accuracy is critical. Therefore two general clinical methods were developed for assessing LLI. Direct methods involve measuring limb length with a tape measure between 2 defined points, in stand. Two common points are the anterior iliac spine and the medial malleolus or the anterior inferior iliac spine and lateral malleolus. Be careful, however, because there is a great deal of criticism and debate surrounds the accuracy of tape measure methods. If you choose for this method, keep following topics and possible errors in mind. Always use the mean of at least 2 or 3 measures. If possible, compare measures between 2 or more clinicians. Iliac asymmetries may mask or accentuate a limb length inequality. Unilateral deviations in the long axis of the lower limb (eg. Genu varum,?) may mask or accentuate a limb length inequality. Asymmetrical position of the umbilicus. Joint contractures. Indirect methods. Palpation of bony landmarks, most commonly the iliac crests or anterior iliac spines, in stand. These methods consist in detecting if bony landmarks are at (horizontal) level or if limb length inequality is present. Palpation and visual estimation of the iliac crest (or SIAS) in combination with the use of blocks or book pages of known thickness under the shorter limb to adjust the level of the iliac crests (or SIAS) appears to be the best (most accurate and precise) clinical method to asses limb inequality. You should keep in mind that asymmetric pelvic rotations in planes other than the frontal plane may be associated with limb length inequality. A review of the literature suggest, therefore, that the greater trochanter major and as many pelvic landmarks should be palpated and compared (left trochanter with right trochanter) when the block correction method is used.
Non Surgical Treatment
After the leg length discrepancy has been identified it can be categorized in as structural or functional and appropriate remedial action can be instigated. This may involve heel lifters or orthotics being used to level up the difference. The treatment of LLD depends on the symptoms being experienced. Where the body is naturally compensating for the LLD (and the patient is in no discomfort), further rectifying action may cause adverse effects to the biomechanical mechanism of the body causing further injury. In cases of functional asymmetry regular orthotics can be used to correct the geometry of the foot and ground contact. In structural asymmetry cases heel lifts may be used to compensate for the anatomic discrepancy.

grow taller supplements
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Mortons Neuroma Overview
 Morton's neuroma is the common name given to the nerve irritation that is found in the ball of the foot that may or may not be accompanied by an inter-metatarsal bursae (a bursa-neuromal complex). It is often associated with inflammation or degeneration and often occurs with constant pressure or irritation of the nerve from the surrounding bony structures or local bursas (fluid filled sacs). Morton's Neuroma can cause symptoms such as a sharp pain, burning even a lack of feeling in the ball of the foot and associated toes.
Morton's neuroma is the common name given to the nerve irritation that is found in the ball of the foot that may or may not be accompanied by an inter-metatarsal bursae (a bursa-neuromal complex). It is often associated with inflammation or degeneration and often occurs with constant pressure or irritation of the nerve from the surrounding bony structures or local bursas (fluid filled sacs). Morton's Neuroma can cause symptoms such as a sharp pain, burning even a lack of feeling in the ball of the foot and associated toes.Causes
Morton's neuroma seems to occur in response to irritation, pressure or injury to one of the nerves that lead to your toes. Factors that appear to contribute to Morton's neuroma include. High heels. Wearing high-heeled shoes or shoes that are tight or ill fitting can place extra pressure on your toes and the ball of your foot. Certain sports. Participating in high-impact athletic activities such as jogging or running may subject your feet to repetitive trauma. Sports that feature tight shoes, such as snow skiing or rock climbing, can put pressure on your toes. Foot deformities. People who have bunions, hammertoes, high arches or flatfeet are at higher risk of developing Morton's neuroma.
Symptoms
Symptoms of interdigital neuroma typically manifest as a sharp, burning or tingling sensation in the forefoot. The pain radiates toward the lesser toes and is aggravated by shoe wear. The pain is relieved when the shoe is removed and the forefoot is massaged. Sometimes the symptoms involve specific toes.
Diagnosis
Your health care provider can usually diagnose this problem by examining your foot. A foot x-ray may be done to rule out bone problems. MRI or ultrasound can successfully diagnose the condition. Nerve testing (electromyography) cannot diagnose Morton neuroma. But it may be used to rule out conditions that cause similar symptoms. Blood tests may be done to check for inflammation-related conditions, including certain forms of arthritis.
Non Surgical Treatment
Most non-operative treatment is usually successful, although it can take a while to figure out what combination of non-operative treatment works best for each individual patient. Non-operative treatment may include the use of comfort shoe wear. The use of a metatarsal pad to decrease the load through the involved area of the plantar forefoot. A period of activity modification to decrease or eliminate activities, which maybe exacerbating the patient?s symptoms. For example, avoiding long periods of standing or other activities that result in significant repetitive loading to the forefoot can be very helpful. Wearing high heels should be avoided. Local corticosteroid injections can help decrease inflammation associated with the nerve. However, this does not necessarily address the underlying loading forces that maybe causing the injury to the nerve in the first place. It has been proposed that an alcohol injection in and around the nerve will cause a controlled death to the nerve and subsequently eliminate symptoms from the nerve. In theory, this may be helpful. In practice, adequate prospective studies have not demonstrated the benefit of this procedure above and beyond the other standard non-operative treatments available. In addition there is the concern that the alcohol will cause excessive scarring and death of other important structures in the area.
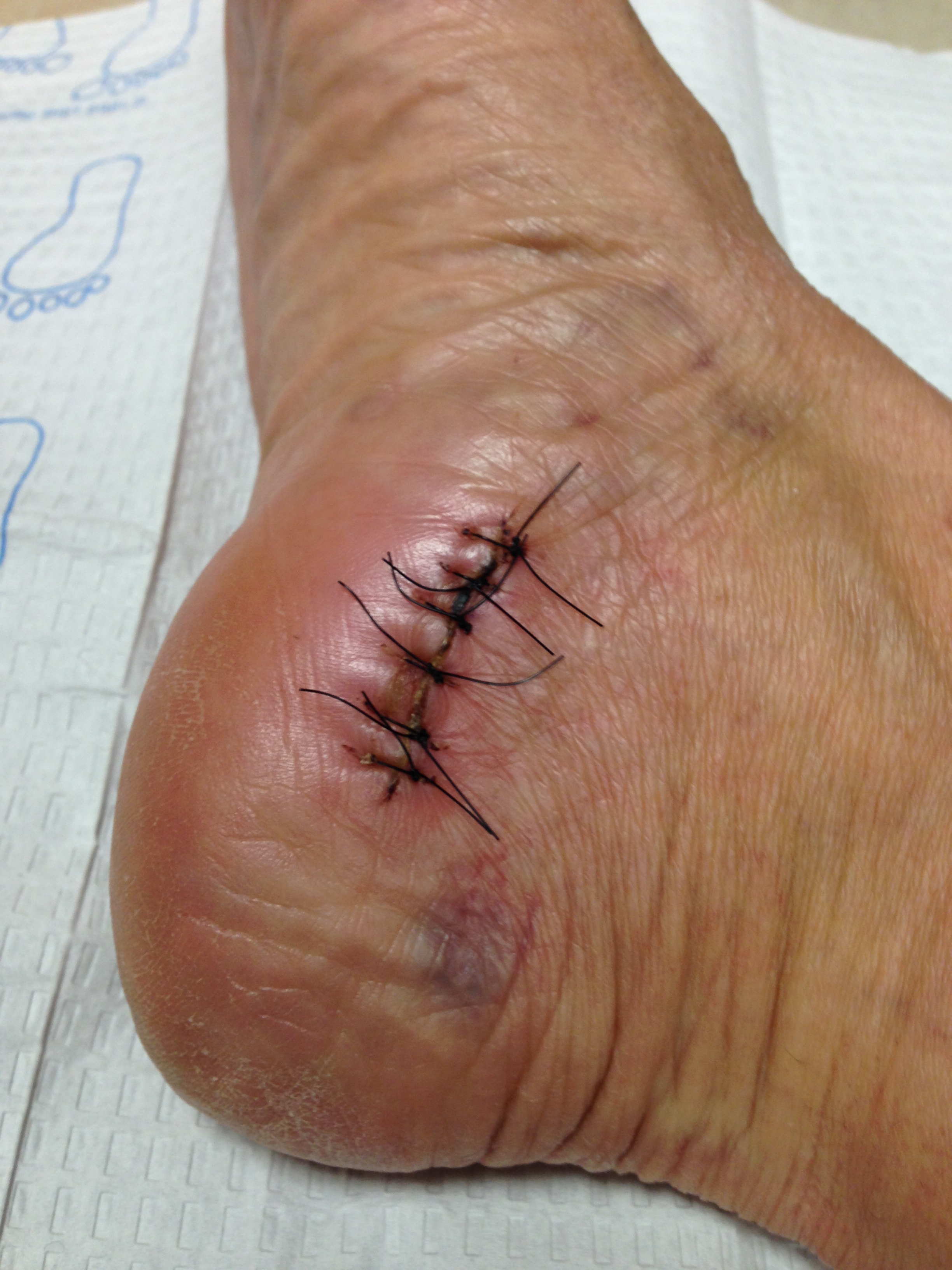
Surgical Treatment
When medications or other treatments do not work, podiatric surgery may be required. The most common surgical procedure for treating Morton?s neuroma is a neurectomy, in which part of the nerve tissue is removed. Although this procedure effectively removes the original neuroma, sometimes scar tissue known as a stump neuroma forms at the site of the incision. This may result in tingling, numbness, or pain following surgery. Surgery is effective in relieving or reducing symptoms for Morton?s neuroma patients in about 75% to 85% of all cases. Occasionally, minimally invasive radio frequency ablation is also used to treat Morton's neuroma.
Prevention
Wearing proper footwear that minimizes compression of the forefoot can help to prevent the development of and aggravation of a Morton's neuroma.
Why Shoe Lifts Are The Best Solution To Leg Length Difference

Leg length inequality goes typically undiscovered on a daily basis, yet this condition is easily solved, and can eradicate quite a few cases of low back pain.
Treatment for leg length inequality typically consists of Shoe Lifts. Most are economical, generally priced at below twenty dollars, in comparison to a custom orthotic of $200 or maybe more. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Upper back pain is easily the most widespread condition afflicting men and women today. Around 80 million people have problems with back pain at some stage in their life. It is a problem that costs employers millions of dollars yearly on account of time lost and productivity. New and more effective treatment solutions are always sought after in the hope of minimizing the economic influence this issue causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In these types of situations Shoe Lifts can be of beneficial. The lifts are capable of relieving any pain in the feet. Shoe Lifts are recommended by numerous expert orthopaedic doctors.
So that you can support the body in a well-balanced manner, feet have a crucial task to play. Despite that, it's often the most neglected area of the body. Some people have flat-feet which means there is unequal force placed on the feet. This will cause other areas of the body like knees, ankles and backs to be affected too. Shoe Lifts ensure that appropriate posture and balance are restored.
Hammer Toe Cosmetic Surgery
 Overview
Overview
Hammertoes are another forefoot deformity that can take a walker out of their activity. A hammertoe generally represent a tendon imbalance in the toes caused by one of the toe tendons getting an advantage over another toe tendon. Most commonly, it is one or all of the long extensor tendons on the top of the foot that gets an advantage over one or all of the flexor tendons on the bottom of the foot, to cause the first joint in the toe to be elevated above the ground. Most shoe wearing people chronically alter the delicate balance that co-exists amongst the toe tendons whether they know it or not.
Causes
If a foot is flat (pes planus, pronated), the flexor muscles on the bottom of the foot can overpower the others because a flatfoot is longer than a foot with a normal arch. When the foot flattens and lengthens, greater than normal tension is exerted on the Hammer toes flexor muscles in the toes. The toes are not strong enough to resist this tension and they may be overpowered, resulting in a contracture of the toe, or a bending down of the toe at the first toe joint (the proximal interphalangeal joint) which results in a hammertoe. If a foot has a high arch (pes cavus, supinated), the extensor muscles on the top of the foot can overpower the muscles on the bottom of the foot because the high arch weakens the flexor muscles. This allows the extensor muscles to exert greater than normal tension on the toes. The toes are not strong enough to resist this tension and they may be overpowered, resulting in a contracture of the toe, or a bending down of the toe at the first toe joint (the proximal interphalangeal joint) which results in a hammertoe.
 Symptoms
Symptoms
Common reasons patients seek treatment for toe problems are toe pain on the knuckle. Thick toe calluses. Interference with walking/activities. Difficulty fitting shoes. Worsening toe deformity. Pain at the ball of the foot. Unsightly appearance. Toe deformities (contractures) come in varying degrees of severity, from slight to severe. The can be present in conjunction with a bunion, and develop onto a severe disfiguring foot deformity. Advanced cases, the toe can dislocate on top of the foot. Depending on your overall health, symptoms and severity of the hammer toe, the condition may be treated conservatively and/or with surgery.
Diagnosis
Most health care professionals can diagnose hammertoe simply by examining your toes and feet. X-rays of the feet are not needed to diagnose hammertoe, but they may be useful to look for signs of some types of arthritis (such as rheumatoid arthritis) or other disorders that can cause hammertoe.
Non Surgical Treatment
There are many non-surgical treatments to help relieve symptoms of hammertoe. The first step for many people is wearing the right size and type of shoe. Low-heeled shoes with a boxy or roomy toe area are helpful. Cushioned insoles, customized orthopedic inserts, and pads can provided relief as well. Splints or straps may be used to help correct toe position. Your doctor may show you toe stretches and exercises to perform. Your doctor can safely remove corns and calluses. You should not try to remove them at home.
Surgical Treatment
In more advanced cases of hammer toe, or when the accompanying pain cannot be relieved by conservative treatment, surgery may be required. Different types of surgical procedures are performed to correct hammer toe, depending on the location and extent of the problem. Surgical treatment is generally effective for both flexible and fixed (rigid) forms of hammer toe. Recurrence following surgery may develop in persons with flexible hammer toe, particularly if they resume wearing poorly-fitted shoes after the deformity is corrected.
 Prevention
Prevention
If you notice signs of hammertoes in your feet, try some of these suggestions. Look for shoes with flat heels and plenty of space to allow your toes to stretch and spread. We're proud to say that all of our shoes at Soft Star feature these qualities. If you're unwilling to give up your heels, at least try to minimize how much you wear them. Instead of wearing heels every day, is it possible to save them for more special occasions? Giving your feet a break from time to time can do wonders. Practice picking up a towel by grabbing it with your toes. You can also try picking up small objects, such as dice. Doing this several times a day can help stretch and strengthen your toe muscles. Show Your Feet Some Love. Getting a foot massage and stretching your calves can help loosen muscles and improve circulation.
New Hammer Toe Surgery
 Overview
Overview
There are two different types of Hammer toes. Flexible Hammer Toes. These hammer toes are less serious because they can be diagnosed and treated while still in the developmental stage. They are called flexible hammer toes because they are still moveable at the joint. Rigid Hammer Toes. This variety is more developed and more serious than the flexible condition. Rigid hammer toes can be seen in patients with severe arthritis, for example, or in patients who wait too long to seek professional treatment. The tendons in a rigid hammer toe have become tight, and the joint misaligned and immobile, making surgery the usual course of treatment.
Causes
Hereditary and shoe gear are probably the most likely reasons to develop a hammer toe. Tight pointy shoes may cause a hammer toes. High heels also can cause hammer toes. A deformed toe often develops over time, and certain types of feet may be predisposed. Some patients may develop a hammer toe or cross over toe (of the 2nd toe) due to a bunion of the big toe. 
Symptoms
The symptoms of hammertoe include a curling toe, pain or discomfort in the toes and ball of the foot or the front of the leg, especially when toes are stretched downward. Thickening of the skin above or below the affected toe with the formation of corns or calluses. Difficulty finding shoes that fit well. In its early stages, hammertoe is not obvious. Frequently, hammertoe does not cause any symptoms except for the claw-like toe shape.
Diagnosis
Some questions your doctor may ask of you include, when did you first begin having foot problems? How much pain are your feet or toes causing you? Where is the pain located? What, if anything, seems to improve your symptoms? What, if anything, appears to worsen your symptoms? What kind of shoes do you normally wear? Your doctor can diagnose hammertoe or mallet toe by examining your foot. Your doctor may also order X-rays to further evaluate the bones and joints of your feet and toes.
Non Surgical Treatment
The treatment options vary with the type and severity of each hammertoe, although identifying the deformity early in its development is important to avoid surgery. Podiatric medical attention should be sought at the first indication of pain and discomfort because, if left untreated, hammertoes tend to become rigid, making a nonsurgical treatment less of an option. Your podiatric physician will examine and X-ray the affected area and recommend a treatment plan specific to your condition.
Surgical Treatment
Surgery may be the treatment of choice if conservative approaches prove unsuccessful. Usually performed as an outpatient procedure, the specific surgery will depend on the type and extent of injury to the toe. Recovery my take several days or weeks and you may experience some redness, stiffness and swelling of the affected toe. Your physician will recommend taking it easy and to keep your foot elevated while you recover.